pISSN : 3058-423X eISSN: 3058-4302
Open Access, Peer-reviewed

pISSN : 3058-423X eISSN: 3058-4302
Open Access, Peer-reviewed
Hoon Choi,Dong Hyun Shim,Min Sung Kim,Bong Seok Shin,Chan Ho Na
10.17966/JMI.2021.26.3.77 Epub 2021 October 04
Abstract
Cutaneous cryptococcosis is classified either as localized cutaneous cryptococcosis, in which the lesions are confined to one area of the skin, or as disseminated cryptococcosis, in which cutaneous manifestations are more widespread. We report a case of fatal disseminated cryptococcosis with characteristic cutaneous manifestations. An 84-year-old woman with diabetes presented with crusted plaques and ulcers that were painful, diffuse, and erythematous to crusted and on only the left side of her face, neck, and upper chest. She was referred to our hospital from a local clinic, where herpes zoster had been suspected. She had no specific systemic symptoms. Histological examination of the skin lesion revealed granulomatous reactions and purple to reddish encapsulated spores. Cryptococcus neoformans was identified in fungal culture, and hospitalization was recommended. Oral fluconazole was prescribed, and she was admitted to another hospital. After 2 weeks, the patient's condition deteriorated, and she was transferred to our hospital. C. neoformans antigen was detected in the blood and urine during the evaluation for systemic involvement. The patient was treated with intravenous amphotericin B and fluconazole; however, she died 10 days after admission. Cutaneous manifestations of disseminated cryptococcosis can appear in various forms and mimic molluscum contagiosum, Kaposi's sarcoma, and cellulitis. In this case, the skin lesions occurred on only the left side of the face, neck, and chest, as in herpes zoster. Cutaneous cryptococcosis can occur before the onset of symptoms of systemic involvement; therefore, diagnosis is important. Systemic evaluation may reveal early markers of disseminated cryptococcosis.
Keywords
Cryptococcus neoformans Cutaneous cryptococcosis Herpes zoster
Cryptococcosis is an invasive fungal infection caused by Cryptococcus organisms, which have a large polysaccharide capsule1. Two species, Cryptococcus neoformans and Crypto- coccus gatti, cause most cases of Cryptococcus in humans. C. neoformans has a universal distribution and is found in natural habitats such as pigeon excreta, decaying wood, hay, and dust. Two variants are classified according to serotype: C. neoformans variety neoformans and C. neoformans variety grubii. C. gatti is found mainly in tropical and subtropical regions in the leaves, bark, and fruit of trees1. Clinical mani- festations of infection vary from asymptomatic pulmonary involvement to a fatal systemic disseminated form. Crypto- coccosis is common in immunocompromised patients and is considered an opportunistic infection. Cutaneous cryptococ- cosis is classified either as localized cutaneous cryptococcosis, in which the lesions are confined within a part of the skin, or as disseminated cryptococcosis, in which cutaneous mani- festations are more widespread and which is reported to occur in 5~15% of all cases of cryptococcosis1-3.
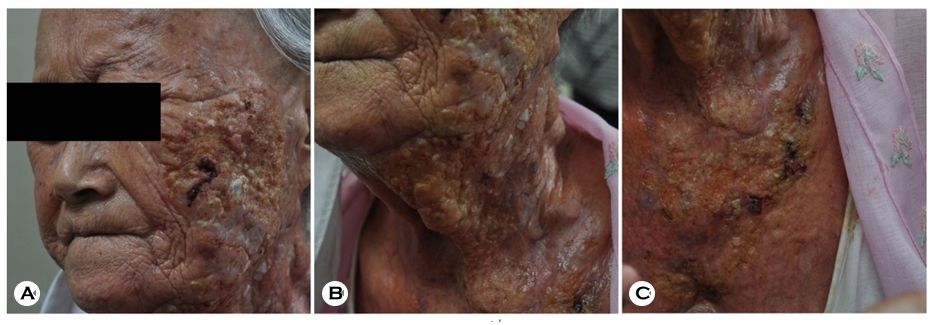
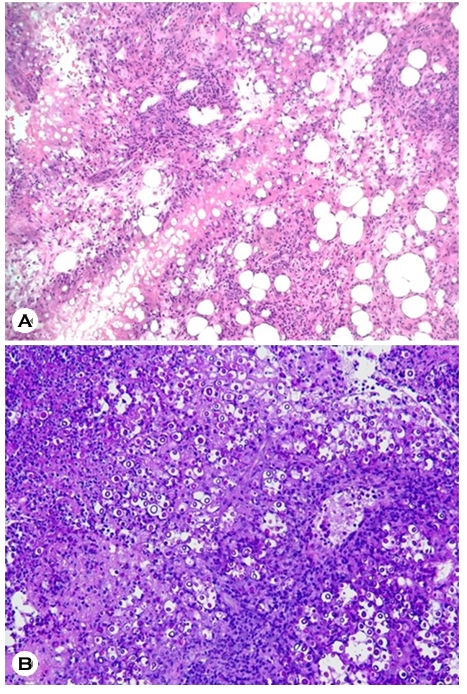
An 84-year-old woman from rural South Korea, who had no history of any other disease except hypertension and uncontrolled diabetes mellitus, presented with painful diffuse erythematous to crusted plaques and ulcers that had been present for 10 days. The skin lesions were unilateral, distributed on only the left side of the face, neck, and upper chest (Fig. 1). The patient was referred to our hospital from a local clinic, where herpes zoster had been suspected. She had no fever, dyspnea, headache, or other systemic symptoms. Bacterial culture, fungal cultures, and punch biopsy were performed. The biopsy specimen was stained with Gomori methenamine silver stain, periodic acid-Schiff (PAS) stain, and acid-fast stain. Spores were observed in the potassium hydroxide test before biopsy, and treatment with itraconazole, 400 mg/day, was initiated under suspicion of a deep fungal infection such as sporotrichosis. Histopathological evaluation revealed a foamy gelatinous and granulomatous appearance with lymphocytes, histiocytes, and giant cells (Fig. 2A). Furthermore, purple to reddish encapsulated spores were also identified with PAS (Fig. 2B). Whitish mucoid colonies were cultured in Sabouraud agar (Fig. 3) and identified as C. neoformans.

Hospitalization was recommended after the diagnosis of C. neoformans infection, but the patient refused. She was prescribed fluconazole, 400 mg/day, and was admitted to another hospital. However, the patient was transferred to our hospital after 2 weeks because the lesions worsened and systemic symptoms, including general weakness, had developed. Complete blood cell count, serum chemistry, and tests for human immunodeficiency virus (HIV) infection yielded no specific findings except an elevation in C-reactive protein level (3.64 mg/dL). Radiologic examinations, including chest radiography and thoracic and brain computed tomo- graphy (CT), and cerebrospinal fluid examinations were performed to evaluate for disseminated cryptococcosis. CT showed underlying interstitial lung disease with pneumonia and pleural effusion. No abnormalities were found in the cerebrospinal fluid (protein level, 33.8 mg/dL; glucose level, 74.8 mg/dL; white blood cell count, 4/μL; C. neoformans antigen: negative) or on brain CT, but blood and urine samples tested positive for C. neoformans antigen. The patient was transferred to the Department of Infectious Diseases and treated with intravenous amphotericin B (30 mg/day) and fluconazole (400 mg/day), but her general condition deteri- orated rapidly. Respiratory failure with fulminant pneumonia, considered to be caused by C. neoformans, developed, and the patient died 10 days after admission.
C. neoformans infection occurs mainly in individuals with impaired immune function, especially those infected with HIV. Other immunocompromizing conditions include malignancy, organ transplantation, long-term use of immunosuppressants, liver cirrhosis, and diabetes mellitus1,4,5. Cryptococcal infection occurs mainly when the fungal spores are inhaled, after which they are deposited in the pulmonary alveoli. Their systemic hematogenous dissemination causes the involvement of organs such as the central nervous system (CNS), kidneys, bone, and skin, especially when immune defensive mechanisms fail1,6. Disseminated cryptococcosis is diagnosed when cultures from at least two different nonadjacent sites or the blood yield positive results, and it is an emergency that necessitates aggressive treatment4,7. The disseminated form can be fatal even with appropriate treatment, as in our patient8. According to a descriptive retrospective study4 of 33 patients with dis- seminated cryptococcosis but without HIV, the mortality rate reached 63%; the most common underlying disease was cirrhosis, followed by diabetes. The uncontrolled diabetes of our patient, in this case, may have rendered her vulnerable to cryptococcal infection.
Cutaneous cryptococcosis can be either primary or sec- ondary, depending on the route of infection. The former, in which infection occurs via the skin, is rarer than the latter, which results from hematogenous transmission. With regard to treatment and prognosis, however, whether the lesion is localized to the skin or systemic can be more important than the route of infection; therefore, a new classification of cutaneous cryptococcosis, localized and disseminated, has been proposed2. Cutaneous manifestations of disseminated cryptococcosis may occur before signs of systemic infection. In a case series study9 of 12 patients with acquired immuno- deficiency syndrome (AIDS) who had cutaneous symptoms of Cryptococcus infection, all had systemic involvement, but three had no symptoms of systemic involvement. In a retro- spective study10 of 30 patients with AIDS-related cryptococ- cosis, cutaneous symptoms occurred several weeks before the first onset of neurologic and systemic symptoms in three of eight patients with cutaneous involvement. The skin symptoms in our patient are also considered manifestations of disseminated cryptococcosis before the onset of symptoms of systemic involvement. Therefore, cutaneous manifestations of cryptococcosis can be an early marker of systemic involve- ment and a clue to diagnosis. Even with CNS involvement, symptoms may be asymptomatic or mild5; therefore, once cutaneous cryptococcosis is diagnosed, patients must be evaluated rapidly for systemic involvement, and appropriate treatment must be instituted immediately.
The diagnosis of cutaneous cryptococcosis can be delayed or challenging because its morphologic features are clinically diverse; they include papules, plaques, nodules, pustules, and ulcers6,9. Umbilicated papules are one of the most common forms and may resemble molluscum contagiosum9-11. Mul- tiple violaceous papules and plaques may resemble Kaposi's sarcoma; abscess and swelling clinically mimic cellulitis and panniculitis6; and herpetiform vesicles12 around the lips have also been reported. The skin lesions are most commonly distributed on the face and neck, and lesions may be both solitary and multiple, but the latter is more common9,12. In our patient, the skin lesions were unilateral, on the left side of the face, neck, and chest; this manifestation was similar to that of herpes zoster, which includes multiple dermatomes. Because of this clinical diversity, clinicians should be alert for features similar to those of cutaneous cryptococcosis and should not hesitate to conduct microscopy, culture, and biopsy for differentiation if it is suspected.
Mild cryptococcosis that does not involve the CNS can be treated with fluconazole, 400 mg daily, for 6~12 months. In contrast, disseminated cryptococcosis necessitates aggressive treatment. The induction regimen for disseminated crypto- coccosis in the absence of HIV infection is amphotericin B with or without 5-fluorocytosine for 2~4 weeks1,7,13. If 5-fluorocytosine is not available, oral or intravenous fluconazole may be used in combination with amphotericin B1. Sub- sequently, fluconazole (400~800 mg/day) should be admin- istered for 8 weeks as consolidation therapy and followed by maintenance therapy with fluconazole, 200 mg/day, for 6~12 months13.
In conclusion, cutaneous manifestations of disseminated cryptococcosis can have a unilateral zosteriform distribution; patients with such skin lesions must be evaluated for systemic involvement even if they have no symptoms once cryptococcal infection is diagnosed.
References
1. Negroni R. Cryptococcosis. Clin Dermatol 2012;30:599-609
2. Noguchi H, Matsumoto T, Kimura U, Hiruma M, Kusuhara M, Ihn H. Cutaneous Cryptococcosis. Med Mycol J 2019; 60:101-107
Google Scholar
3. Futatsuya T, Anzawa K, Mochizuki T, Shoji A, Hoshino Y, Abe M. Disseminated cutaneous cryptococcosis in an immunocompetent elderly long-term pigeon fancier. J Dermatol 2020;47:551-553
Google Scholar
4. Chuang YM, Ho YC, Chang HT, Yu CJ, Yang PC, Hsueh PR. Disseminated cryptococcosis in HIV-uninfected patients. Eur J Clin Microbiol Infect Dis 2008;27:307-310
Google Scholar
5. Kim SW, Jung SI, Kim YS, Ki HK, Kim CK, Kim S, et al. Cryptococcal meningitis in 25 non-AIDS patients. Korean J Infect Dis 1999;31:467-473
Google Scholar
6. Hayashida MZ, Seque CA, Pasin VP, Enokihara MMSES, Porro AM. Disseminated cryptococcosis with skin lesions: report of a case series. An Bras Dermatol 2017;92:69-72
Google Scholar
7. Yang Y, Shen YN, Zong WK, Cui PG. Disseminated crypto- coccosis. Indian J Dermatol Venereol Leprol 2016;82:206-208
Google Scholar
8. Maleb A, Hami A, Lahlou YB, Lamrabat S, Rifai S, Rahmani N, et al. Disseminated Cryptococcosis Incorrectly Managed: a Case Report. J Mycol Infect 2019;24:28-31
Google Scholar
9. Murakawa GJ, Kerschmann R, Berger T. Cutaneous Cryptococcus infection and AIDS. Report of 12 cases and review of the literature. Arch Dermatol 1996;132:545-548
Google Scholar
10. Manfredi R, Mazzoni A, Nanetti A, Mastroianni A, Coronado O, Chiodo F. Morphologic features and clinical significance of skin involvement in patients with AIDS-related cryptococcosis. Acta Derm Venereol 1996;76:72-74
Google Scholar
11. Ghigliotti G, Carrega G, Farris A, Burroni A, Nigro A, Pagano G, et al. Cutaneous cryptococcosis resembling molluscum contagiosum in a homosexual man with AIDS. Report of a case and review of the literature. Acta Derm Venereol 1992;72:182-184
Google Scholar
12. Borton LK, Wintroub BU. Disseminated cryptococcosis presenting as herpetiform lesions in a homosexual man with acquired immunodeficiency syndrome. J Am Acad Dermatol 1984;10:387-390
Google Scholar
13. Perfect JR, Dismukes WE, Dromer F, Goldman DL, Graybill JR, Hamill RJ, et al. Clinical practice guidelines for the management of cryptococcal disease: 2010 update by the Infectious Diseases Society of America. Clin Infect Dis 2010;50:291-322
Google Scholar
Congratulatory MessageClick here!