pISSN : 3058-423X eISSN: 3058-4302
Open Access, Peer-reviewed

pISSN : 3058-423X eISSN: 3058-4302
Open Access, Peer-reviewed
Jisoo Kim,Joonsoo Park
10.17966/JMI.2023.28.3.61 Epub 2023 October 06
Abstract
Malassezia infection and candidiasis are commonly encountered in dermatology clinics and need to be differentiated from other fungal infections or skin diseases. These can be diagnosed by a simple test, such as the KOH procedure, and can be appropriately treated to relieve patient discomfort. In this article, we reviewed the diseases caused by Malassezia (i.e., pityriasis versicolor and Malassezia folliculitis) and various superficial skin infections caused by Candida.
Keywords
Candidiasis Malassezia Malassezia folliculitis Pityriasis versicolor
Malassezia (Pityrosporum) yeast is a lipophilic fungus that has been associated with dermatologic diseases, such as pityriasis (tinea) versicolor and Malassezia folliculitis, as well as in inflammatory skin diseases, such as seborrheic dermatitis and atopic dermatitis. However, the role of Malassezia in these dermatologic diseases had been unclear and thought to be more of an aggravating factor rather than a real fungus infection. Malassezia is known to be part of the normal flora of the skin of humans and mammals1. In humans, colony formation increases immediately after birth, while the activity of the sebaceous glands increases2, and peaks during puberty and adulthood. Particularly, colonization tends to occur at 3~6 months after birth or earlier with prolonged neonatal intensive care unit stay.
Malassezia skin infections, such as pityriasis versicolor and Malassezia folliculitis, occur at high rated in tropical regions and with heavy sweating. In addition, immunosuppression and intake of oral antibiotics or corticosteroids had been the associated risk factors for Malassezia folliculitis. Notably, there is no sex difference in the incidence rate of Malassezia follic- ulitis. There are currently 14 species in the genus of Malassezia; of which, 11 species have been detected as human normal skin flora. Malassezia globosa had been the most frequently isolated species in both pityriasis versicolor and Malassezia folliculitis, but Malassezia restricta and Malassezia sympodialis were also frequent in Malassezia folliculitis.
Skin diseases, such as pityriasis versicolor, Malassezia follic- ulitis, and seborrheic dermatitis, are known to be caused by the disruption of the normal skin barrier and other immune actions3. In addition, the association among diseases, such as atopic dermatitis, acne vulgaris, psoriasis, confluent and reticulated papillomatosis, and Malassezia onychomycosis have been reported. Moreover, Malassezia has been found to play a key role in other diseases, such as chronic rhinosinusitis, urinary tract infection, meningitis, pneumonia, nosocomial bloodstream infection, and catheter-related fungemia.
Malassezia skin infections are usually harmless, and most respond easily to appropriate antifungal therapy. However, recurrence is common, particularly in individuals with strong risk factors. Preterm babies, immunosuppressed patients, and patients on parenteral lipid infusions are at a relatively high risk of disseminated infection. Among the representative diseases caused by Malassezia infection, the dermatologic conditions pityriasis versicolor and Malassezia folliculitis are described here.
2.1 Introduction and symptoms
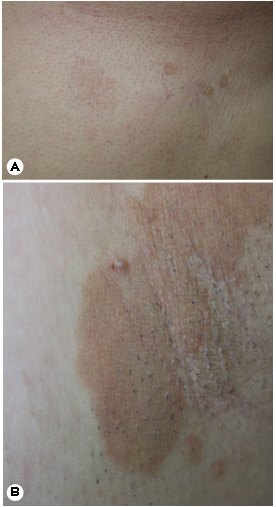
Pityriasis versicolor, which is also known as tinea versicolor, is a superficial Malassezia infection of varying sizes and is commonly seen in adolescents and young adults (i.e., 20~ 30 years age group)4. Pityriasis versicolor may present in a spectrum, from being asymptomatic to mildly pruritic patches and thin plaques with overlying fine scales (Fig. 1A). The commonly affected areas are the neck, chest, back, upper arms, and, less commonly, the scalp, abdomen, and inguinal areas. These areas have abundant sebaceous glands, and lesions are sometimes fused5. As the term versicolor suggests, the affected area may have color changes, including hypo- pigmentation and hyperpigmentation, as well as erythematous to salmon-colored (i.e., yellow ocher to reddish brown) scaly patches. It often appears during hot and humid summer seasons, progresses chronically, worsens in summer, and improves in autumn and winter.
2.2 Diagnosis
The characteristic cutaneous morphology is the most important finding for the diagnosis of pityriasis versicolor (Fig. 1B). When illuminated with a wood lamp, a yellow-green fluorescence is emitted, and shiny fine needles can be seen on dermoscopy6,7. Dermoscopy has been recommended as an additional tool for confirming the diagnosis of pityriasis versicolor, because it highlights the fine scaling, which may not always be readily visible to the naked eye. A KOH mount is particularly useful for the diagnosis of Malassezia in the clinics. After dropping a 1:1 mixture of 20% KOH solution and Parker ink on the collected scales, short hyphae and round spores in the shape of spaghetti and meatballs can be seen8. Fungal culture can be performed on a glucose peptone agar medium, with an appropriate amount of fat added after inoculation. However, fungal culture is not routinely used to diagnose Malassezia infection. On histological examination, Malassezia yeast forms and hyphae can be observed on the thick reticulated stratum corneum.
2.3 Differential diagnosis
The differential diagnoses of pityriasis versicolor include seborrheic dermatitis, pityriasis rosea, pityriasis alba, tinea corporis, impetigo, secondary syphilis, mycosis fungoides, atopic dermatitis, irritant contact dermatitis, and allergic con- tact dermatitis. Therefore, if pityriasis versicolor is suspected, care must be taken to not confuse it with these other conditions through accurate history taking and appropriate diagnostic tests.
2.4 Treatment
The first line treatment choices are topical agents and shampoos. Ketoconazole is the best known and widely used topical azole antifungal cream, but the other options are imidazole, triazoles, selenium sulfide, ciclopirox olamine, zinc pyrithione, sulfur preparations, salicylic acid preparations, propylene glycol in aqueous solution, and benzoyl peroxide9. If lesions are extensive or do not respond well to topical agents, oral itraconazole 200~400 mg/day for 3~7 days or fluconazole 300 mg twice daily for 1 week may be tried10,11; the latter may be preferable because of its more variable bioavailability. Oral ketoconazole was once a mainstay of therapy but is no longer recommended because of the risk of liver and adrenal damage. Oral terbinafine exhibits lower efficacy, compared with itraconazole or fluconazole.
Notably, complete eradication of the hypo- or hyperpig- mentation changes, particularly the hypopigmented patches, in Malassezia, may take long. Therefore, patients should be counseled about appropriate expectations and receive explan- ations on the possibility of persistent depigmentation long after treatment and that this is not a sign of treatment failure. Because Malassezia is a normal part of the skin microbiome, it is difficult to eliminate by treatment, and recurrence is common. Given the high possibility of recurrence, prophy- lactic use of appropriate agents may be recommended in some patients. These prophylactic agents include periodic use of topical selenium sulfide shampoo or 2% ketoconazole shampoo or oral intake of itraconazole 200 mg twice daily once a month for 6 months.
3.1 Symptoms
Malassezia folliculitis, which is also known as pityrosporum folliculitis, is characterized by follicularly based erythema- tous monomorphic papules and pustules on the face; trunk, particularly the upper body; and upper arms or shoulder, which are locations with increased sebaceous gland activity. The lesions are sometimes pruritic. Malassezia folliculitis is frequently misdiagnosed as acne vulgaris and may appear concurrently with acne. It occurs frequently in immunosup- pressed patients, such as those who have undergone organ or bone marrow transplant.
3.2 Diagnosis
Malassezia folliculitis can be diagnosed clinically; by a yellow-green fluorescence upon wood lamp irradiation, direct micro- scopy, and culture findings of yeast; and by the response to antifungal agents. Although superficial scarping of skin scales is adequate for the diagnosis of pityriasis versicolor, the use of a comedone extractor or a needle to puncture an intact pustule is recommended to obtain a specimen for the diag- nosis of Malassezia folliculitis. In Malassezia folliculitis, the yeast is situated deeper within the follicle. On histopath- ological examination, yeast forms and hyphae may be seen within the hair follicle and the surrounding dermis. There may be perivascular inflammatory infiltrates of lymphocytes, histiocytes, and neutrophils; these are typically mild, unless the follicle has ruptured. A periodic acid-Schiff (PAS) stain can be used to highlight the organism.
3.3 Differential diagnosis
The differential diagnoses of Malassezia folliculitis include acne vulgaris, bacterial folliculitis, steroid folliculitis, eosinophilic folliculitis, and rosacea. Care should be taken to diagnose it accurately and to not confuse it with these other conditions, using clinical symptoms and appropriate diagnostic tests as the basis.
3.4 Treatment
Malassezia spp. colonizes the deep tissues within the hair follicle, and topical antifungal agent monotherapy is less effective. Treatment with keratolytic agents, such as propylene glycol, may improve the efficacy of topical antifungal treat- ment. Eventually, many patients require systemic treatment, and if the lesion is extensive, itraconazole 200 mg per day for 1~3 weeks may be prescribed12. Recurrence is common and may require topical antifungal agents for prophylaxis13.
Candidiasis is a disease caused by Candida albicans or other fungi of the same genus and can infect the skin, nails, mucous membranes, and internal organs14. C. albicans is the most common and most pathogenic causative organism, but other species, such as Candida glabrata, Candida tropicalis, Candida krusei, Candida parapsilosis, Candida dubliniensis, Candida guilliermondii, Candida lustinaniae, and Candida kefyr, had also been identified and are potentially pathogenic. Candida strains are part of the normal flora of the skin; oropharyngeal, respiratory, and gastrointestinal tract; genital area; and mucous membranes, but opportunistic superficial cutaneous Candida infection may occur because of various factors that lower the immune function of a host15. Moreover, Candida spp. can sometimes present as a life-threatening disseminated disease, such as candidemia. The typical risk factors of candidiasis include old age, intake of immunosuppressants, pregnancy, diabetes mellitus, obesity, burn, and use of broad-spectrum antibiotics.
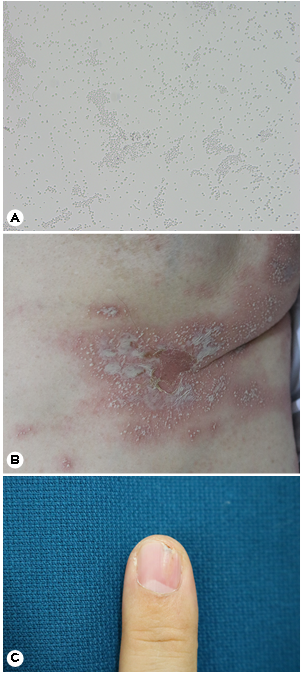
The diagnosis is made by considering both clinical symptoms and laboratory findings. The characteristic morphology is important to make a clinical diagnosis of superficial Candida skin infection. On direct microscopy, a mixture of KOH solu- tion and Parker ink is dropped to confirm the presence of sausage-shaped pseudohyphae with constricted connections and long hyphae with uniform width and budding. In addition, Candida yeast can be seen on direct microscopy (Fig. 2A). When inoculated and cultured on Sabouraud agar medium, cream-colored or white colonies are observed. Although not routinely done, a skin biopsy may be necessary to make a definitive diagnosis of candidiasis. In the epithelium or stratum corneum, Candida may be easily seen with Grocott methe- namine silver or PAS staining. The differential diagnoses of cutaneous candidiasis include seborrheic dermatitis, tinea corporis, impetigo, intertrigo, irritant contact dermatitis, and allergic contact dermatitis.
The general and important considerations in the treatment of candidiasis include isolation from infectious agents, cor- rection of immunocompromised disorders, and administration of antifungal agents. The affected area should be kept dry and clean, and the oral cavity, including dentures, should be cleaned. Patients usually respond well to topical antifungal agents, but oral antifungal agents are used for mouth lesions in patients with acquired immunodeficiency syndrome (AIDS), esophageal infection, the prevention of systemic spread in neutropenic patients, onychomycosis, chronic mucocutaneous candidiasis, or deep-infected candidiasis.
In the field of dermatology, we look at the representative diseases that appear as cutaneous and mucosal candidiasis and the treatment options for these.
2. Thrush
Thrush or acute pseudomembranous candidiasis is a grayish-white film that comprises exfoliated epidermal cells, fungal elements, inflammatory cells, and fibrin and is observed on the mucosal surface. It most commonly appears within the first week of life and is often seen in patients with immuno- deficiency, such as AIDS. The other risk factors are diabetes mellitus and old age. The differential diagnoses of oral can- didiasis include herpes simplex virus infection, oral hairy leukoplakia, lichen planus, and white sponge nevus. Topical antifungal agents can be used as first line treatment. Nystatin suspension had been mainly used for newborns16, and clotri- mazole lozenge (Troche) can be used for adults. Fluconazole or itraconazole can be administered in cases of reinfection and chronic infections.
3. Candidal intertrigo
In this condition, itching, erythema, and soreness occur in the intertriginous areas, such as the genital region, thigh, axilla, gluteal fold, and lower breast; satellite vesicles or pustules may be irregularly distributed around these areas (Fig. 2B). The risk factors include obesity, diabetes, tight clothing, and exposure to water or moisture17. The differential diagnoses are tinea corporis, seborrheic dermatitis, and Hailey-Hailey disease. Topical agents, such as nystatin and imidazole cream, are effective, but recurrence is common. A topical steroid mixture may help relieve symptoms quickly.
4. Diaper candidiasis
Diaper candidiasis in infants is caused by Candida, which originates from the gastrointestinal tract and spreads to the buttocks and genitals because of prolonged diaper use. There may be intercutaneous rashes with irregular edges and satellite lesions that start around the anus and spread to the perineum. Similar to candidal intertrigo, topical application of nystatin or imidazole cream is effective for diaper candidiasis.
5. Perianal candidiasis
In this condition, erythema, exudation, and soreness with severe itching and burning sensation appear around the anus. Because Candida may spread to abnormal tissues, such as that seen in extramammary Paget’s disease, a biopsy may be necessary in cases that are refractory to treatment18.
6. Candidal vulvovaginitis
It is a common condition that affects approximately two-thirds of women at least once in their lifetime. C. albicans commonly inhabits the vagina but may cause severe itching, burning sensation, and discharge when there is overgrowth. There may be visible turbid erythema, curd-like milky white stains, or simple erythema on the vaginal mucosa and labia. The discharge may vary in consistency from watery to whitish-thick. This condition occurs frequently in pregnancy, diabetes, oral contraceptive use, and broadspectrum antibiotic intake. Long-term tamoxifen treatment is known to be associated with recurrent candidal vulvovaginitis. For acute vulvovaginitis, imidazole cream and vaginal tablets are used for 3~7 days; oral fluconazole or itraconazole can also be used19.
7. Candidal balanitis
This lesions comprise small papules or papular pustules on the glans penis and can rupture to form shallow erythema- tous erosions with white scales. The factors that can trigger candidal balanitis are candidal vulvovaginitis in the partner and diabetes. Therefore, simultaneous treatment of the sexual partner and treatment of predisposing factors, such as dia- betes, are necessary. In cases of widespread lesions, long-term persistence, or recurrence, a urine glucose test is essential. The treatment is topical application of clotrimazole cream several times a day or oral administration of fluconazole 150 mg once a day.
8. Angular cheilitis or perleche
Secondary infection of C. albicans or Staphylococcus aureus results in the characteristic outward and downward fissure formation in the labial commissures. Painful sores on one or both corners of the lips appear with ulcers, crusts, and triangular erythema. It mostly affects elderly individuals who wear dentures and may be seen in patients with riboflavin deficiency, anorexia nervosa, Down syndrome, oral candidiasis, diabetes, and AIDS. The topical application of nystatin and hydrocortisone is effective, and mupirocin ointment is used for a confirmed S. aureus infection.
9. Candidal paronychia and onychomycosis
Paronychia is characterized by painful invasion of the nail, reddish and swollen nail folds, and loss of the nail cuticle (Fig. 2C). Most cases of acute paronychia are caused by Staphylococcus infection, but chronic paronychia is caused by various factors, such as Candida spp., bacteria, or irritant or allergic contact dermatitis. Peripheral circulatory disorders are common in many patients, particularly in treatment-resistant cases. The management includes avoidance of irritants and moist environments, application of imidazole lotion, and improvement of peripheral circulation. If topical treatment fails, oral fluconazole or itraconazole may be effective.
The Candida infection usually starts as a paronychia but can also directly invade the nail plate and produce onycho- mycosis. The several presentations of this condition include a distal subungual lesion and total dystrophic onychomycosis. candidal onychomycosis is more often seen in the finger- nails than in the toenails. The risk factors include Cushing's syndrome and Raynaud's phenomenon. The first line therapy for candidal onychomycosis is oral itraconazole for a total minimum duration of 4 weeks for the fingernails and 12 weeks for toenail disease.
In this article, we discussed the spectrum of cutaneous yeast infections caused by Candida and Malassezia, which are frequent commensal organisms in human hosts. Candida behaves as an opportunistic pathogen that manifests as fairly characteristic patterns of skin and mucosal inflammation and nail infection and has the potential to lead to invasive and, sometimes, life-threatening disseminated disease. On the other hand, Malassezia infection presents with several superficial cutaneous patterns and is rarely a culprit in systemic disease.
Malassezia infection and candidiasis are common diseases encountered in dermatology. Like most dermatological dis- eases, these diseases may impair the quality of life and cause discomfort in affected individuals. Therefore, knowing the characteristic symptoms, proper diagnosis, and treatment of each disease can be of great help to patients.
References
1. Marcon MJ, Powell DA. Human infections due to Mala- ssezia spp. Clin Microbiol Rev 1992;5:101-119
Google Scholar
2. Luigi N, Alfredo R. Seborrheic Dermatitis. N Engl J Med 2009;360:387-396
Google Scholar
3. Shibata N, Okanuma N, Hirai K, Arikawa K, Kimura M, Okawa Y. Isolation, characterization, and molecular cloning of a lipolytic enzyme secreted from Malassezia pachydermatis. FEMS Microbiol Lett 2006;256:137-144
Google Scholar
4. Gupta AK, Foley KA. Antifungal treatment for pityriasis versicolor. J Fungi 2015;1:13-29
Google Scholar
5. Chebil W, Haouas N, Chaâbane-Banaoues R, Remadi L, Chargui N, M'rad S, et al. Epidemiology of pityriasis ver- sicolor in Tunisia: Clinical features and characterization of Malassezia species. J Mycol Med 2022;32:101246
Google Scholar
6. Thomas N, Malakar S. Dermoscopy: An easy way to solve the diagnostic puzzle in pityriasis versicolor. Indian J Dermatol Venereol Leprol 2019;85:664-665
Google Scholar
7. Zhou H, Tang XH, De Han J, Chen MK. Dermoscopy as an ancillary tool for the diagnosis of pityriasis versicolor. J Am Acad Dermatol 2015;73:e205-e206
Google Scholar
8. Maleki M, Fata A. Evaluation of Wood's light and direct smear for diagnosis of pityriasis versicolor and erythrasma. Saudi Med J 2005;26:1483-1484
Google Scholar
9. Akabery AA, Amini SS, Hajihosseini H. An unusual form of tinea versicolor: A case report. Iranian J Dermatol 2009; 12:s30-s31
Google Scholar
10. Borelli D. Treatment of pityriasis versicolor with ketoco- nazole. Rev Infect Dis 1980;2:592-595
Google Scholar
11. Ahn KJ, Kim KJ, Yi GJ, Yang KM. Efficacy of one-week regimen of itraconazole for pityriasis versicolor. Korean J Med Mycol 1999;4:124-130
Google Scholar
12. Chae KS, Yoon DH, Lee JD, Lee JY, Kim JW, Cho BK. A case of Malassezia (Pityrosporum) folliculitis associated with pityriasis (tinea) versicolor. Korean J Med Mycol 1997;2:174-177
Google Scholar
13. Marín-Hernández E, Mejía-Mancera CG, Quijada-Henderson MA, Valero-Gómez A. Atypical folliculitis caused by Malassezia spp. in immunosuppressed patients. Bol Med Hosp Infant Mex 2022;79:62-68
Google Scholar
14. Kim OJ, Oral candidiasis. Journal of Korean Dental Asso- ciation 2010;48:355-364
Google Scholar
15. Mohamed AA, Lu XL, Mounmin FA. Diagnosis and treat- ment of esophageal candidiasis: Current updates. Can J Gastroenterol Hepatol 2019:3585136
Google Scholar
16. Yoo DW, Park KD, Kwon HJ, Seo JW, Yoon JH, Kim KH. A case of oral candidiasis treated with fluconazole (Diflucan®) mouthrinse. JMI 2023;28:10-13
Google Scholar
17. Metin A, Dilek N, Bilgili SG. Recurrent candidal intertrigo: challenges and solutions. Clin Cosmet Investig Dermatol 2018;11:175-185
Google Scholar
18. van der Linden M, Meeuwis KA, Bulten J, Bosse T, Poelgeest MI, de Hullu JA. Paget disease of the vulva. Crit Rev Oncol Hematol 2016;101:60-74
Google Scholar
19. Martin Lopez JE. Candidiasis (vulvovaginal). BMJ Clin Evid 2015:0815
Google Scholar
Congratulatory MessageClick here!